- Original Article
- Critical Care Medicine
- Telemedicine outcome of mechanically ventilated children in Brazilian pediatric intensive care units
- Aristóteles de Almeida Pires, Luciano Remião Guerra, João Ronaldo Mafalda Krauzer, Luciane Gomes da Cunha, Mariana Motta Dias da Silva, Vanessa Cristina Jacovas, Hilda Maria Rodrigues Moleda Constant, Taís de Campos Moreira, Paulo Márcio Pitrez, Felipe Cezar Cabral
- Clin Exp Pediatr. 2026;69(2):140-149. Published online October 23, 2025
-
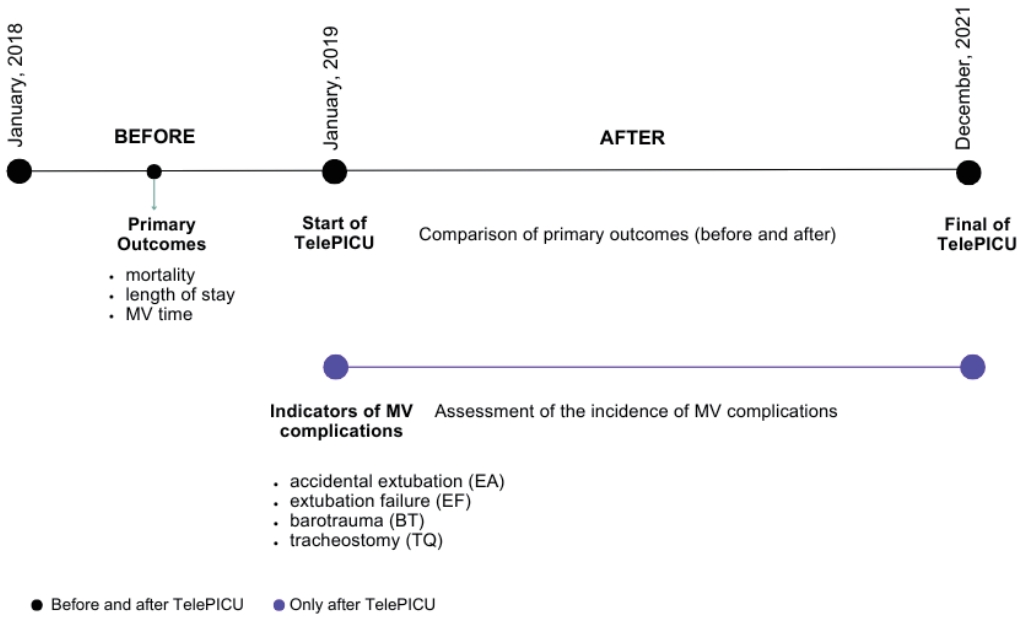
Question: Telemedicine interventions in Brazilian public pediatric intensive care units effectively address the challenges related to specialized care provision in resource-limited settings.
Finding: The implementation of telemedicine significantly reduced overall mortality rates among mechanically ventilated children (from 20.7% to 10.4%) and increased ventilator-free days from 3 (interquartile range, 0–7) to 4 (interquartile range, 2–8) days.
Meaning: These findings support telemedicine as a viable strategy for enhancing pediatric critical care in public health systems, particularly by improving patient outcomes.
- High-dose methylprednisolone and tocilizumab improve survival of patients with high-risk pediatric acute necrotizing encephalopathy
- Chaonan Fan, Fei Li, Kechun Li, Zheng Li, Yiyang Mao, Lijuan Wang, Gang Liu, Yingchao Liu, Quan Wang, Suyun Qian
- Clin Exp Pediatr. 2026;69(1):56-64. Published online October 22, 2025
-

Question: Which immunomodulatory strategies can reduce mortality in children with acute necrotizing encephalopathy (ANE)?
Finding: High-dose methylprednisolone (30 mg/kg/day) significantly improved the survival of high-risk patients, particularly when combined with tocilizumab.
Meaning: These findings support the use of a severity-based immunotherapy approach to optimize the outcomes of pediatric ANE.
- Cytokine profile of Post–cardiopulmonary bypass in children
- Kantara Saelim, Kanokpan Ruangnapa, Jirayut Jarutach, Pongsanae Duangpakdee, Smonrapat Surasombatpattana, Pharsai prasertsan
- Clin Exp Pediatr. 2025;68(12):1015-1022. Published online September 19, 2025
-

Question: Can cytokine levels predict low cardiac output syndrome (LCOS) in children post–cardiopulmonary bypass?
Finding: Elevated interleukin (IL)-6, IL-8, and tumor necrosis factor-α levels were associated with LCOS, with an increase in IL-8 of >56 pg/mL from baseline to immediately postoperative being the strongest predictor.
Meaning: Monitoring immediately postoperative IL-8 levels may help identify pediatric patients at risk of LCOS, enabling timely interventions to improve outcomes.
- Effect of postoperative enteral protein supplementation on nitrogen balance in critically ill children
- Irene Yuniar, Kadek Apik Lestari, Antonius Hocky Pudjiadi, Fatima Safira Alatas, Yoga Devaera
- Clin Exp Pediatr. 2025;68(10):790-800. Published online May 30, 2025
-

Question: Does high-protein enteral nutrition better increase the average nitrogen balance (NB) and decrease the intestinal fatty acid-binding protein (I-FABP) level of critically ill postoperative children than standard-protein enteral nutrition?
Finding: The study demonstrated a significant increase in average NB but no significant decrease in I-FABP levels in the high- versus low-protein group.
Meaning: These findings suggest that high-protein enteral nutrition can improve NB in critically ill postoperative children, thereby supporting their recovery.
- Serum amyloid A and proadrenomedullin as early markers in critically ill children with sepsis
- Nagwan Y. Saleh, Wafaa M. Abo El Fotoh, Mona S. Habib, Salem E. Deraz
- Clin Exp Pediatr. 2025;68(8):578-586. Published online February 26, 2025
-
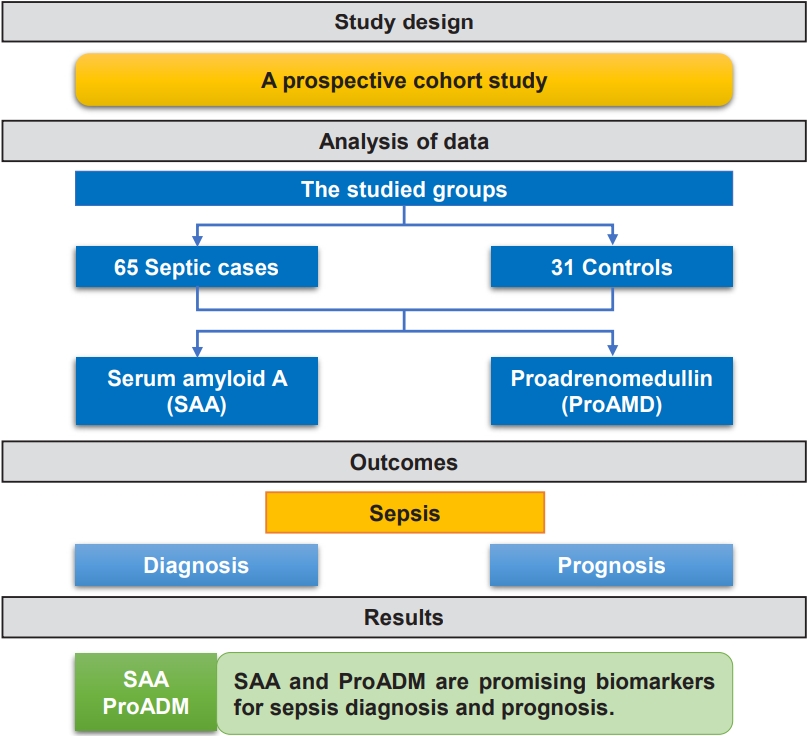
Question: Are serum amyloid A (SAA) and proadrenomedullin (proADM) levels early markers in critically ill children with sepsis?
Finding: This prospective case-control study included 65 critically ill children with sepsis admitted to the pediatric intensive care unit and 31 controls. SAA and proADM levels were significantly higher in patients versus controls.
Meaning: SAA and proADM are promising biomarkers for diagnosing and predicting outcomes in pediatric sepsis.
- Review Article
- Critical Care Medicine
- Protocolized sedation may reduce ventilation and sedation requirements in the pediatric intensive care unit: a systematic review and meta-analysis
- Ambrus Szemere, Alíz Fazekas, Anna Réka Sebestyén, Rani Ezzeddine, Veronika Upor, Marie Anne Engh, Péter Hegyi, Zsolt Molnár, Klára Horváth
- Clin Exp Pediatr. 2025;68(6):406-416. Published online February 19, 2025
-
Protocolized sedation may reduce ventilation requirements, pediatric intensive care unit length of stay, and sedative exposure. However, it may increase the likelihood of unplanned extubation, highlighting the importance of incorporating preventive measures to mitigate this risk.
- Recent updates on systemic treatment of atopic dermatitis
- Jiyoung Ahn
- Clin Exp Pediatr. 2024;67(11):580-588. Published online November 1, 2024
-
Atopic dermatitis (AD) is a complex disease with multifactorial pathogenesis and variable clinical presentation. Up to one-fifth of patients with AD develop moderate to severe disease that is often refractory to classical therapies and can compromise quality of life. This review summarizes recent clinical evidence on biological agents and small-molecule immunotherapies for the treatment of AD.
- Editorial
- Critical Care Medicine
- Is it possible to provide palliative care to pediatric patients with neurological diseases?
- Young-Hoon Kim
- Clin Exp Pediatr. 2024;67(8):403-404. Published online February 15, 2024
-
· Patients with neurological diseases often require external mechanical support to maintain mechanical ventilation or supply.
· Little has been done to help the families of affected children make difficult decisions that carry significant physical and psychological consequences.
· The establishment of a department that provides pediatric palliative care for neurological patients should be considered.
- Original Article
- Critical Care Medicine
- Timing of parenteral nutrition initiation in critically ill children: a randomized clinical trial
- Nagwan Y. Saleh, Hesham M. Aboelghar, Nehad B. Abdelaty, Mohamed I. Garib, Asmaa A. Mahmoud
- Clin Exp Pediatr. 2023;66(9):403-411. Published online June 14, 2023
-

Question: What is the ideal initiation timing of parenteral nutrition for critically ill children?
Finding: This randomized clinical trial of 140 children examined the effects of an early or late start of parenteral nutrition on mechanical ventilation need (primary outcome) and length of stay and mortality (secondary outcomes).
Meaning: Children who received early versus late parenteral nutrition had lower mechanical ventilation need and duration.
- Review Article
- Critical Care Medicine
- Ferritin in pediatric critical illness: a scoping review
- Ivy Cerelia Valerie, Anak Agung Sagung Mirah Prabandari, Dyah Kanya Wati
- Clin Exp Pediatr. 2023;66(3):98-109. Published online September 16, 2022
-
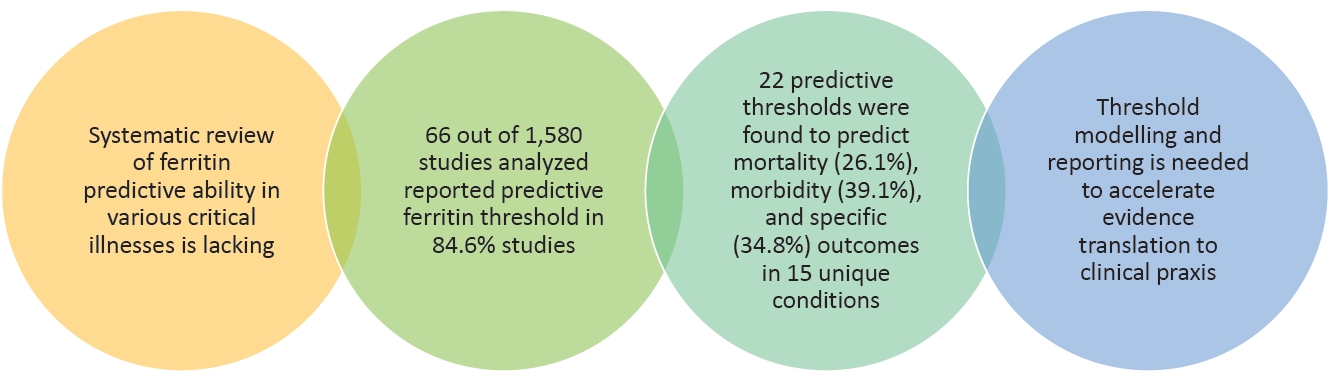
The number of studies on ferritin predictive ability in pediatric critical illness has grown exponentially over the past 2 decades. However, among the 66 of 1,580 studies analyzed here, summary statistics for overall and condition-specific studies were only reported in 45.4% and 71.2%, respectively. In contrast, ferritin as a categorical variable with a preset threshold was a significant predictor in 84.6% of studies.
- Letter to the Editor
- Critical Care Medicine
- Role of serum bilirubin-to-albumin ratio as a prognostic index in critically ill children
- You Min Kang, Ga Eun Kim, Mireu Park, Jong Deok Kim, Min Jung Kim, Yoon Hee Kim, Kyung Won Kim, Myung Hyun Son, Soo Yeon Kim
- Clin Exp Pediatr. 2023;66(2):85-87. Published online December 5, 2022
-
- Review Article
- Critical Care Medicine
- Pediatric postintensive care syndrome: high burden and a gap in evaluation tools for limited-resource settings
- Chanapai Chaiyakulsil, Rapee Opasatian, Paweethida Tippayawong
- Clin Exp Pediatr. 2021;64(9):436-442. Published online December 18, 2020
-

Pediatric postintensive care syndrome has high impact and burden and can affect a child’s life for decades. The early evaluation and detection of such problems require a simple and less time-consuming surveillance tool. Current evaluation tools can be difficult and strenuous for areas with limited resources. Thus, a new simple tool is required for the early detection and intervention of postintensive care syndrome in critically ill children
- The use of extracorporeal membrane oxygenation in children with acute fulminant myocarditis
- Silver Heinsar, Sainath Raman, Jacky Y. Suen, Hwa Jin Cho, John F. Fraser
- Clin Exp Pediatr. 2021;64(5):188-195. Published online August 10, 2020
-

Acute fulminant myocarditis (AFM) occurs as an inflammatory response to an initial myocardial insult. Its rapid and deadly progression calls for prompt diagnosis with aggressive treatment measures. The demonstration of its excellent recovery potential has led to increasing use of mechanical circulatory support, especially extracorporeal membrane oxygenation (ECMO). Arrhythmias, organ failure, elevated cardiac biomarkers, and decreased ventricular function at presentation...
- Original Article
- Critical Care Medicine
- Can central venous access device care bundles and regular feedback reduce central line-associated complications in pediatric patients?
- Chanapai Chaiyakulsil, Onsuthi Pharadornuwat
- Clin Exp Pediatr. 2021;64(3):123-129. Published online July 14, 2020
-
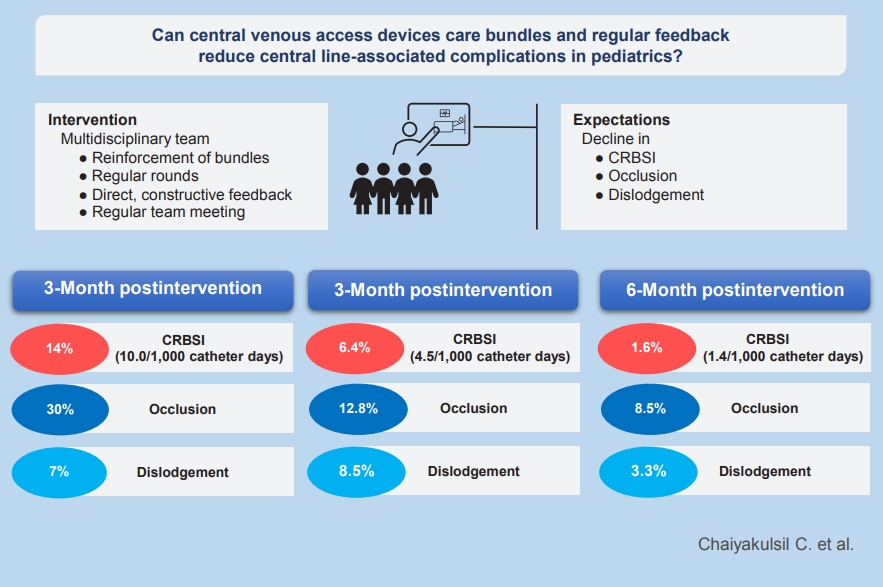
Question: Can central line bundles and feedback reduce central line-associated complications in pediatric patients?
Finding: The central line-related bloodstream infection rate decreased from 10.0 catheter-days to 1.4/1,000 catheter-days at 6-month postintervention. The central line occlusion rate was also decreased.
Meaning: Reinforcing central line care bundles with direct feedback can significantly decrease central line-associated complications in pediatric patients.
- Assessment of interhospital transport care for pediatric patients
- Krittiya Chaichotjinda, Marut Chantra, Uthen Pandee
- Clin Exp Pediatr. 2020;63(5):184-188. Published online August 29, 2019
-

Background: Many critically ill patients require transfer to a higher-level hospital for complex medical care. Despite the publication of the American Academy of Pediatrics guidelines for pediatric interhospital transportation services and the establishment of many pediatric transport programs, adverse events during pediatric transport still occur.
Purpose: To determine the incidence of adverse events occurring during pediatric transport and explore their complications...
- Comparative validity of microalbuminuria versus clinical mortality scores to predict pediatric intensive care unit outcomes
- Shifa Nismath, Suchetha S. Rao, B.S. Baliga, Vaman Kulkarni, Gayatri M. Rao
- Clin Exp Pediatr. 2020;63(1):20-24. Published online August 12, 2019
-
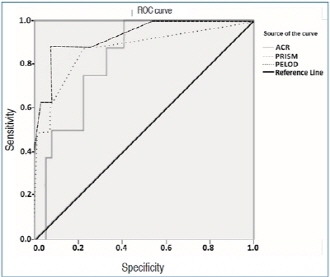
Question: Does microalbuminuria predict mortality in pediatric intensive care unit?
Finding: Positive correlation was found between albumin-creatinine ratio and pediatric intensive care unit stay, organ dysfunction and need of inotropes. Area under the receiver operating characteristic curve for albumin-creatinine ratio was comparable to mortality scores.
Meaning: Microalbuminuria is a good predictor of outcome in pediatric intensive care unit and is comparable with mortality scores.