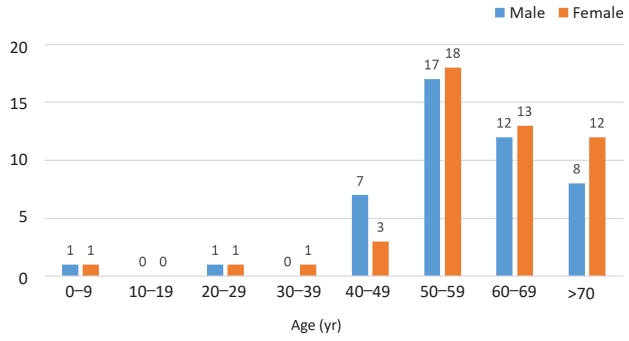
Recent published article entitled “Changes in age-specific seroprevalence of Japanese encephalitis virus and impact of Japanese encephalitis vaccine in Korea” [1] reviewed the recent epidemiologic and seroprevalence changes of Korea. Currently, Japanese encephalitis (JE) cases occur predominantly in adults suspected with unvaccinated against JE vaccine in Korea (Fig. 1).
JE is a mosquito-borne viral disease that occurs throughout most of Asia, parts of the Western Pacific, and northern Australia [2]. JE is one of the most important recognized causes of encephalitis in Asia. Despite the availability of effective vaccines, more than 67,000 JE cases occur annually. About 75% of these cases are children younger than 15 years of age [3]. JE cannot be distinguished from other encephalitis based on clinical presentation, and specific laboratory tests are needed to confirm. Therefore, the exact incidence of JE is likely to be underestimated.
As the transmission dynamics between mosquito vectors, natural hosts, and human continue to evolve, the epidemiology of JE has been changed constantly. Several factors, such as global climate change, changes in agricultural practice, population increase, and effective immunization program, have influenced on the recent epidemiologic changes of JE.
Japanese encephalitis virus (JEV) is transmitted in an enzootic cycle between Culex mosquitoes and pigs, wading birds, and other vertebrates which serve as amplifying hosts. Humans are incidental or dead-end hosts, because they usually do not develop a level of viremia sufficient to infect mosquitoes. Among Culex species, Culex tritaeniorhynchus are primary vectors of JEV [3]. They breed in rice paddy and pools of water. Pigs are mainly raised near home, so they serve as important bridging hosts, bringing the virus to humans. In temperate climate, Culex mosquito emerge usually in May. JEV amplified several times between mosquitoes and pigs. Shortly thereafter, human infections followed, usually from May to September. Because of the mode of transmission, JE has been considered a disease in rural area. However, this article showed that JE cases occurred more frequently in urban or suburban areas nowadays in Korea [1]. The relative risk of JE infection in urban and suburban areas of Korea was similar to rural area. This shift of risk area also has been reported in China, Singapore, and Taiwan [4]. Although reasons for risk area shift to urban or suburban area are not clear, improvement of rice cultivation methods, segregation of pigs from human residence, rapid urbanization, and other environmental factors may effect on this epidemiological change. Studies conducted in Japan and Korea suggest that migratory birds such as egrets and herons may be responsible for human JE cases of urban area [5,6]. Future studies regarding sero-epidemiology and virus genotyping in migratory birds will be needed to verify the role of migratory birds in terms of transmission of JEV in urban area in Korea.
In addition to risk area shift of JE, age shift is clearly observed in countries with high JE vaccination rates in children such as Japan [7], Taiwan [8], and Korea [1]. In Taiwan, the main age group of JE shifted to adults over 30 years old after 2001. Since JE vaccine was introduced in 1968, JE immunization schedules have changed frequently in Taiwan. As a result, various birth cohorts had received different doses of the JE vaccine. The cohort born between 1963 and 1975 received just 2 or 3 doses of the vaccine and only 54% of the cohort have seropositive against JEV. A JE surveillance study conducted in Japan from 1982 to 2004 also revealed that JE mainly occurred in unvaccinated populations over 40 years of age. Providing vaccination targeting unvaccinated adult could be considered as a policy to reduce adult JE cases in these countries. Unlike Japan and Taiwan, 2 recent seroepidemiology studies conducted in Korea showed the seropositive rate had maintained at an appropriate level in adults [9,10]. Multiple JE epidemics and mandatory annual JE vaccination for all children aged 3–15 years from 1985 to 1995 could contribute to maintaining of a high positive rate of antibody against JE. Therefore, the necessity of immunization of unvaccinated adults to reduce the incidence of JE is likely to be low in Korea at present.
The recent epidemiologic changes of JE in Korea paradoxically show the importance of vaccination against JE in children. The near elimination of JE in children can be attributed primarily to the high rates of JE vaccination in children. Because elimination of JE is expected to be impossible based on the enzootic transmission cycle, high vaccination rates should be maintained to keep the near elimination status in all age groups. The JE vaccines currently used in Korea seem to maintain immunity for several years, but the exact duration of longterm immunity is still not well known. To determine number of booster doses for childhood JE immunization, the need for targeted vaccination to unvaccinated adults or routine booster dose for adults, surveillance for mosquito vectors, human JE cases, and seroprevalence should be carried out continuously.





 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link PubMed
PubMed Download Citation
Download Citation


