Implication of microRNA as a potential biomarker of myocarditis
Article information
Abstract
Myocarditis was previously attributed to an epidemic viral infection. Additional harmful reagents, in addition to viruses, play a role in its etiology. Coronavirus disease 2019 (COVID-19) vaccine-induced myocarditis has recently been described, drawing attention to vaccine-induced myocarditis in children and adolescents. Its pathology is based on a series of complex immune responses, including initial innate immune responses in response to viral entry, adaptive immune responses leading to the development of antigen-specific antibodies, and autoimmune responses to cellular injury caused by cardiomyocyte rupture that releases antigens. Chronic inflammation and fibrosis in the myocardium eventually result in cardiac failure. Recent advancements in molecular biology have remarkably increased our understanding of myocarditis. In particular, microRNAs (miRNAs) are a hot topic in terms of the role of new biomarkers and the pathophysiology of myocarditis. Myocarditis has been linked with microRNA-221/222 (miR-221/222), miR-155, miR-10a*, and miR-590. Despite the lack of clinical trials of miRNA intervention in myocarditis yet, multiple clinical trials of miRNAs in other cardiac diseases have been aggressively conducted to help pave the way for future research, which is bolstered by the success of recently U.S. Food and Drug Administration-approved small-RNA medications. This review presents basic information and recent research that focuses on myocarditis and related miRNAs as a potential novel biomarker and the therapeutics.
Key message
· Myocarditis was recently examined quantitatively as inflammation of the heart muscle based on endomyocardial biopsy, and its noninvasive diagnosis remains unsatisfactory.
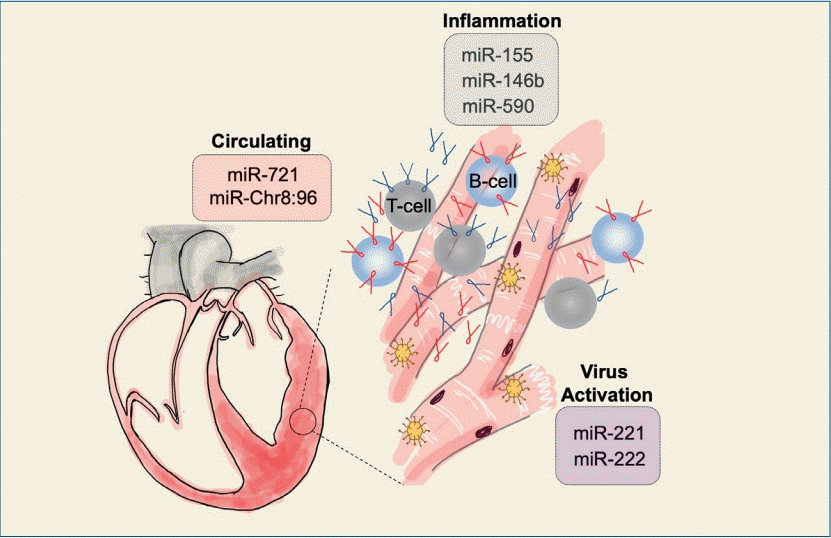
· Additionally, numerous miRNAs (miR-155, miR-146b, miR-590, miR-221, miR-222, etc.) coupled with inflammation or viral activation have been examined in myocarditis patients or mouse models.
· The recent identification of mmu-miR-721 (has-miR-Chr8: 96), a myocarditis-specific microRNA, demonstrated its potential as an acute myocarditis biomarker.
Graphical abstract.
Introduction
Myocarditis is a broad term for inflammatory disorders of the heart muscles. In his work, Traité des Maladies du Coeur (Treatise on Heart Disease) published in 1749, Jean Baptiste Senac identified inflammation in the heart. Later, Joseph Freidrich Sobernheim coined the term myocarditis to describe cardiomyopathy caused by myocyte inflammation, ischemia, and hypertensive heart disease [1]. Various viral infections in the heart, such as coxsackievirus, echovirus, the mumps virus, influenza virus, measles virus, poliovirus, and smallpox, have been reported during epidemic periods, leading to myocarditis becoming a broader term that covers myocardial infarction, chronic ischemic heart disease, and occasionally, pancarditis or myopericarditis [2,3]. To date, it has been used interchangeably. Recent efforts have been made to clearly describe myocarditis, which is defined as inflammation of the cardiac muscle and recognized as a disease that leads to heart failure [1,4].
Endomyocardial biopsy (EMB) with quantitative standards (≥14 lymphocytes/mm2, including ≤4 monocytes/mm2, with the presence of cluster of differentiation 3–positive T lymphocytes, 7 cells/mm2) and immunohistochemistry assays are used to diagnose myocarditis [3,5]. However, this approach is only acceptable for isolated inflammatory regions, making it difficult to diagnose fulminant myocarditis (FM), which involves widespread inflammation throughout the heart [6,7]. Quantitative cardiac troponin analysis combined with cardiac magnetic resonance imaging (MRI) to assess the injured myocardium can be utilized to noninvasively diagnose myocarditis to overcome localized inflammation, spontaneous resolution, and myocardium sampling difficulties [8-11].
According to the International Classification of Illnesses 9th revision, myocarditis affects approximately 22 per 100,000 individuals worldwide [12,13]. Systematic reviews of the clinical courses of myocarditis patients from the Lombardy registry (443 patients from the Italian region) and 220 cases in 2018, which used combined diagnostic strategies, revealed that left ventricular systolic dysfunction, ventricular arrhythmias, hemodynamic instability, and QRS width should be considered the initial diagnostic factors for FM [14,15].
An estimated, 0.5%–4 % of myocarditis cases progress to heart failure [13]. Myocarditis, which is the leading cause of sudden death among young athletes, is particularly prevalent, accounting for 5%–12% of all deaths [16]. Furthermore, our understanding of the etiology of myocarditis is limited, although we know that it can occasionally resolve spontaneously or result in heart failure, highlighting the need for early diagnosis and accurate comprehension [4].
This review presents basic information and recent research highlights in the field of myocarditis, with a particular focus on disease-specific microRNA (miRNA) expression patterns and the goal of their potential use as alternative prognostic and diagnostic tools to supplement the current standards.
Myocarditis etiology
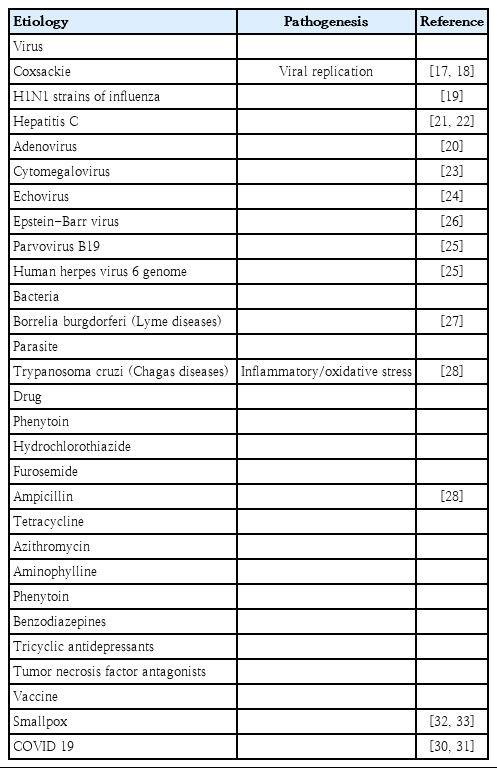
Infection, autoimmune responses, and toxicity are the 3 most common causes of myocarditis. Among them, viral infections are the most common. Several viruses, including coxsackievirus [17,18], H1N1 influenza [19], adenovirus [20], hepatitis C [21,22], cytomegalovirus [23], echovirus [24], parvovirus B-19, herpes virus [25], and Epstein-Barr virus [26] were detected in heart autopsy samples on a regular and local basis [26]. In addition to viral infectionmediated immune responses, bacterial-driven cases such as Lyme disease (Borrelia burgdorferi) [27] and parasite-mediated Chagas disease (Trypanosoma cruzi) [28] have been reported regularly, as have drug- or vaccine-related cases such as ampicillin or tetracycline [29-31] or smallpox vaccines [32,33].
Amid the recent coronavirus disease 2019 (COVID-19) pandemic, cases of myocarditis reported in people vaccinated with the COVID-19 mRNA vaccine and the relationship between myocarditis after COVID-19 infection and vaccination are under investigation. This finding was supported by 2 major cohort studies. One survey in Israel reported 136 cases of definitive or probable myocarditis within one month of receiving one shot of the vaccine. This study included more than 5 million participants who had received immunization. Of these cases, 135 had a mild or moderate clinical course and one was fatal. After the second dose of the vaccination, a 15 in 100,000 chance of developing myocarditis was assessed in adolescents and young men aged 16–19 years [30]. Similar studies in the United States reported a somewhat lower rate of 5 of 10,000 cases (18- to 24-year-old men). However, all of these cases were less severe than myocarditis caused by direct viral infection. Severe acute respiratory syndrome coronavirus 2 infection results in an 18fold increased risk of myocarditis in the same age group [31].
Two 10-year studies of Koreans included cases of myocarditis in children. Park et al. [34] studied the incidence of myocarditis in Korean children in 2010–2019. This multicenter study included 142 patients with myocarditis/pericarditis. The patients were a mean 5.4 years of age, with males accounting for 61% of the total. Compared to other age groups ranging from 17 days to 17 years of age, the teen years, defined as ages 12–17 years, had the highest prevalence of 1.25 per 1,000 patients. The frequency of occurrence has increased considerably over the last decade from 0.34 in 2010 to 1.25 in 2019. Among the principal etiologies of infections are Mycoplasma pneumoniae, enterovirus, rhinovirus, adenovirus, respiratory syncytial virus, influenza virus, parainfluenza virus, and parvovirus. On rare occasions, adenoviruses and endemic coronaviruses have been observed simultaneously. However, in 60% of patients, no pathogens were detected. Between 2007 and 2016, another study enrolled 1,462 pediatric cases after health insurance evaluations. The annual occurrence has increased from 1.4 to 2.1. Male patients over the age of 13 years were much more numerous in the 2010–2019 survey [35]. The incidence of myocarditis is bimodal, with peaks during infancy and midadolescence, similar to the 2 peaked cardiac growth signals [36,37]. These 2 studies reported a similar trend of myocarditis in Korean children: (1) Its proclivity for growth continues to increase annually; and (2) In midadolescence, boys are more prone to its development.
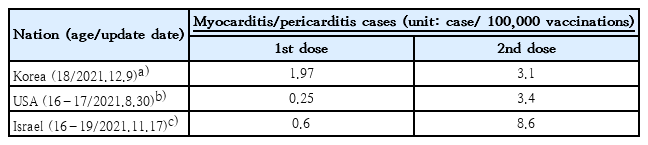
In Korea, COVID-19 vaccinations for third-year high school students began in July 2021. The incidence of myocarditis was calculated. Myocarditis occurred in 1.97 of every 100,000 cases after the first dose and 3.1 of every 100,000 cases after the second dose per 100,000 vaccine cases. These data were provided concurrently with the incidence in the United States and Israel based on a report from Korea’s Disease Control and Prevention Agency (12-9-21 release). According to this report, myocarditis cases in Korea are approximately 7 times higher than that described in the United States or 3 times more than that in Israel for the first dose. However, the incidence after the second immunization dose was comparable to or lower than that of other 2 countries. Notably, Israel’s incidence following the second dose is 2.77 times higher than that in Korea. Table 1 illustrates a three-nation comparison focusing on midadolescent age cases of the myocarditis after vaccinations.
Myocarditis pathogenesis
Because viral infection is the most common cause of myocarditis, viral infection-mediated pathology is discussed here. These studies are mostly based on the pathophysiological understanding of the murine model. The first step is linked to viral replication in the heart, resulting in cellular rupture, an antigenindependent and innate immune response. Consequently, adaptive immune responses are triggered in antigen-presenting cells, resulting in the production of antigen-specific antibodies. Autoimmune reactions and cellular damage propagate during this stage as cardiac proteins are released through cardiomyocyte rupture. Finally, the replacement of collagen with dead myocardium results in persistent inflammation and fibrosis [38].
There is also disagreement regarding whether viral infection is a direct pathogenic cause of cardiac injury. It is a situation in which a virus triggers immune responses to cause cardiomyocyte injury, or that cardiomyocyte injury is caused by viral infection. The presence of the viral genome in the myocardium of patients with chronic inflammatory cardiomyopathy, rather than acute myocarditis, is suggested [39,40]. Reports on FM associated with viral infection frequently adopted nasopharyngeal swabs for the diagnosis of viral infection [41]. The hs-troponin level was also elevated in COVID-19 patients, suggesting that the virus generated aberrant immune-mediated inflammatory responses rather than viral-directed myocyte damage [42-44]. Understanding the pathophysiology, whether the virus is directly or indirectly involved, is critical for immunosuppression because its role is also conflicting [3,45]. The use of immunosuppressive medication should generally be validated by polymerase chain reaction to ensure that the condition is not an active infection in EMB [3].
Patients with acute myocarditis alone or in combination with autoimmune responses were also identified among those who received immuno-checkpoint inhibitor (ICI) medications [46,47]. Since many cancer patients have just begun to utilize ICI treatment and its estimated correlation with myocarditis is 1.14%, it may become a subtype of myocarditis with distinct age and inflammatory type in the near future [46].
Myocardial inflammation and the cellular compartment
Idiopathic, autoimmune, and infectious are the 3 types of myocardial inflammation [4]. Interactions between several cellular compartments causes myocardial inflammation. T-, B-, and lymphoid-derived cells, such as macrophages, dendritic cells, granulocytes, mast cells, and immature precursor cells, all contribute to the differentiation of inflammatory cells and myofibroblasts [4]. Caspase-1, n-terminal PYRIN PAAD DAPIN and c-terminal caspase-recruitment domain containing, and nucleotide-binding oligomerization domain-like receptor pathways play a role in the production of proinflammatory cytokines during this process. Toll-like receptors (TLRs) have also been implicated in the activation of innate immune responses in the early stages [48]. TLR3 polymorphism have been linked to enteroviral myocarditis [49]. Tumor necrosis factor-α (TNF-α) and interleukin (IL)-1β are also released in the myocardium by the TLR pathway [50,51].
Inflammatory cell invasion is aided by macrophages. Because Ly6Chi inflammatory macrophages are found in the early stages of cardiac damage, their blockade has been used to treat autoimmune myocarditis [52-54]. The Ly6Clow M2 macrophage is a critical factor in the transition from acute to pathological remodeling via myofibroblast replacement [55,56]. Thymic resistance to alpha-myosin heavy chain (MyHC) causes, at least in part, T-cell function to quell autoimmune responses after clearing infections [57,58]. Overexpressing alpha-MyHC promoterspecific T-cell receptors were designed for a mouse autoimmune myocarditis model based on this understanding [59]. The release of cytokines by T cells determines myocarditis progression. T-helper (Th) type 1 cells produce interferon gamma, while Th2 cells produce IL-4, -5, and -13. Type 17 helper T (Th17) cells mainly produce IL-17 [60-63].
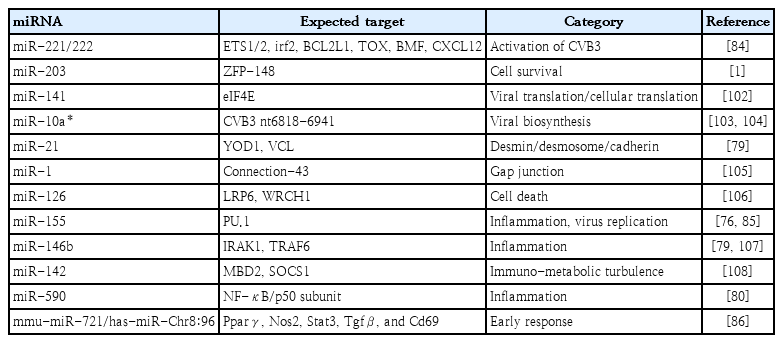
While lymphoid-derived cells are involved in adaptive immune responses, endothelial cells act as barriers preventing circulating bone marrow-derived cells from entering the heart. Interstitial cell types, such as fibroblasts, myofibroblasts, and stromal cells, act as a matrix to modify the inflammatory phenotype via local cues. During pathogenesis, the cardiomyocyte compartment is also involved in early infection and adaptive responses such as altered calcium signaling or hypertrophy [64,65]. Both direct and indirect cross-talk was used to orchestrate these interactions (Table 2) [66].
Myocarditis and miRNA
There has been research on the posttranscriptional modulation of cardiac immunological responses, including miRNA-mediated controls. MiRNAs are 22-nt single-strand RNAs that complementarily base pair with mRNAs, primarily but not exclusively in the 3′ untranslated region, to govern translation by a minimum 6-mer base-pairing. This is generally a translational repressor [67,68].
The importance of miRNAs in myocardial specification and cardiac development, as well as in cardiac disorders such as cardiac hypertrophy, myocardial infarction, arrhythmia, myocarditis, coronary artery disease, and heart failure, has been recognized [69-71]. Circulating miRNAs in the blood have been used to identify novel biomarkers in addition to their role in the heart [72,73]. MED13 and miR-208a are 2 of the most notable regulators of metabolic homeostasis via systemic control [74]. Table 3 summarizes the miRNAs in heart disorders, including myocarditis.
Several miRNA profiling studies have been conducted. A total of 107 miRNAs were dysregulated in human right ventricular myocarditis samples [75]. The inhibition of miR-155, miR-21, and miR-146b, for example, reduced cardiac inflammation and myocardial damage in a coxsackievirus B3 (CVB3) animal model and mouse autoimmune studies [76-79]. Furthermore, miR-590-3p overexpression reduced disease by repressing nuclear factor kappa B (NF-κB) expression and turning off IL-6/TNF-α expression by targeting NF-κB [80].
Patients with myocarditis were profiled for various CVB3 clearance conditions. Patients with defective cardiac function under protracted viral accumulation (CVB3) had a greater expression of 8 miRNAs, including miR-135b, -155, -190, -422a, -489, -590, -601, and -1290 [81]. Circulating miRNAs in the blood have been investigated as a means of diagnosis or prognosis, while myocarditis is present. miR-208 and miR-499 were overexpressed in the blood plasma during acute myocarditis. However, misregulation of these 2 miRNAs has been documented in acute ischemia and hypertensive disorders, implying that other defining factors may be required [82,83]. Cellular release in response to inflammation could explain the mixed expression of these 2 miRNAs [82].
In mouse myocarditis model studies involving enterovirus CVB3, the dysregulation of miR-221/222 by targeting ETS1/2, interferon regulatory factor 2, and B-cell lymphoma 2 (Bcl2)like-11 maintained prolonged cardiac viremic states and activate inflammatory and injury pathways by targeting ETS1/2, interferon regulatory factor 2, and Bcl2-like-11 [84]. MiR-155 uses a similar regulatory mechanism to activate immune responses such as T cells and monocytes by targeting PU.1 and suppressor of cytokine signaling 1 [84,85].
Recent studies using a murine myocarditis model revealed the induction of cardiac myosin-specific Th17 lymphocytes in a myocarditis-specific manner, turning on as early as 3 days after onset, which differs from the response of myocardial infarction, which also showed Th17 cell upregulation later in the disease course. Using a murine model, the authors validated Th17 cell upregulation of mmu-miR-721 from 27 dysregulated miRNAs. The authors stated that dysregulation of the human version of miR-721, has-miR-Chr8:96, was confirmed in a large human cohort study that included 42 myocarditis patients (based on cardiac MRI diagnosis), 90 myocardial infarction patients, and 80 healthy participants, implying that it could be used as a biomarker for acute myocarditis [86].
A total of 113 miRNAs were differentially expressed in a murine myocarditis model using Trypanosoma cruzi. The authors reported that miR-146b, miR-21, miR-142-3p, miR-142-5p, miR-145-5p, and miR-149-5p were correlated with disease severity [79].
MiRNAs as medications for cardiac diseases
Although antisense RNAs as a novel mechanism for medication have been explored since 1978 [87], the success of partisiran, a short RNA drug that mimics siRNAs with pharmacological features to treat polyneuropathy, has only recently become beneficial for treatment [88-90].
Small RNA therapies, either inhibiting or activating, are likely to be actively developed for the medical intervention of heart disorders [90-93]. In the pharmaceutical industry, there are 2 primary types of antitechnologies that repress miRNAs. The first is antagomir [94], a cholesterol-based modified RNA, while the second is locked nucleic acid (LNA)-modified RNA [70, 95]. AntimiR-92a, also known as MRG-110, is an LNA/DNA mixed, phosphorothiorate linkage, and 16-nucleic acid medication that was administered intravenously and had a repressive efficacy of up to 2 weeks with a single dose in healthy humans [96]. Taubel et al. [97] used an antisense LNA method to block miR-132-3p in patients with heart failure. This group previously demonstrated that LNA-based chemical modification approaches effectively lowered miRNA levels while maintaining Watson-Crick basepairing [98].
Furthermore, scientists demonstrated that miR-132-3p repression clearly improved the heart failure mouse model [99], which was then expanded into a large animal setting as a preclinical trial to determine the dosage with enhanced cardiac functions [100]. With this excellent research background, the authors assessed the efficacy of LNA-miR-132-3p (CDR132L) for the first time by examining heart failure biomarkers, cardiac fibrosis, QRS narrowing, and left ventricular ejection fraction. For 28 patients, 4 dosage groups with a maximum dose of 10 mg/kg administered every 4 weeks were created. Efficacy assessments were underpowered in the phase 1b trial due to the research design and small patient cohort, but this study clearly demonstrated the safety of a dose-dependent reduction of plasma miR-132-3p expression level and encouraged the next stage in the development of this innovative drug [97].
MiRNAs as biomarkers for cardiac diseases
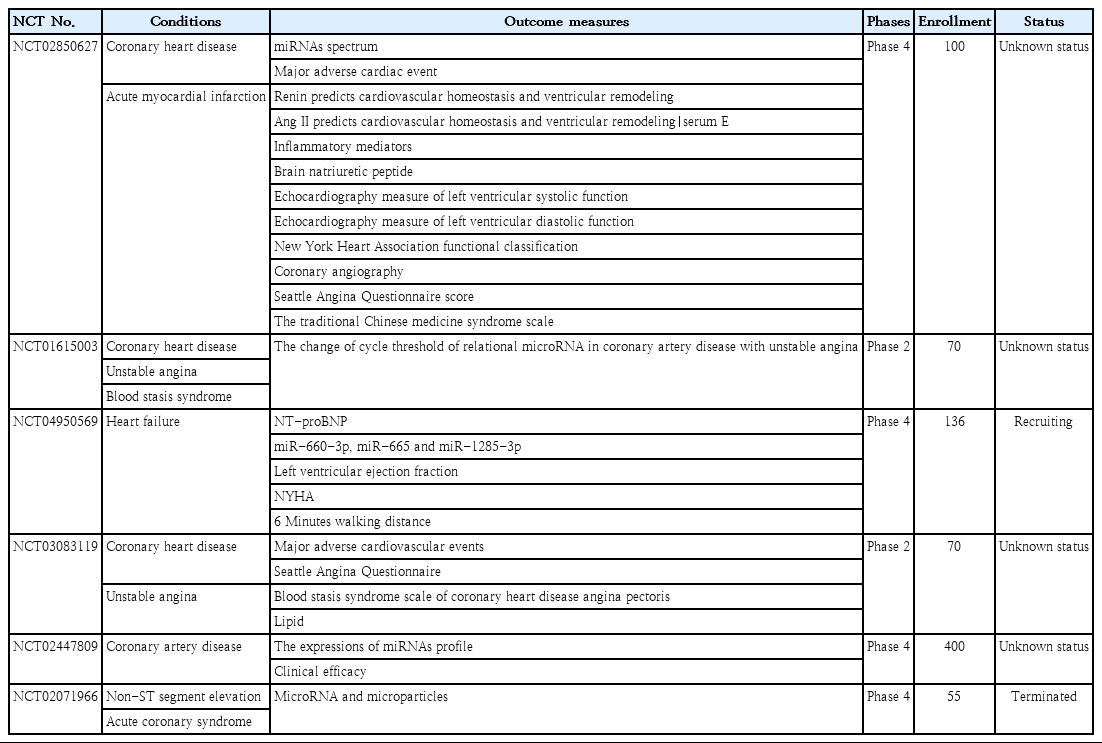
In both experimental animals and humans, miRNA expression profiling has been shown to reflect disease status and/or progression. Misregulation of miR-195 and miR-21 was observed for the first time in mouse models of heart hypertrophy [101]. Since then, a large amount of miRNA profiling data has been amassed in various cardiovascular disease models and patients, leading to current active clinical trials [73]. In heart failure patients, for example, profiling miRNA expression as biomarkers from patients receiving U.S. Food and Drug Administration (FDA)–approved medications has been described. Table 4 contains detailed information on miRNA investigations in clinical trials.
Conclusion
Myocarditis remains a challenge, and the recent COVID-19 outbreak has brought it back to the forefront. Although its exact pathophysiology remains unknown, new research is seeking to improve our understanding and lay the groundwork for newer treatment methods. MiRNAs offer further insights into this understanding.
Notes
Conflicts of interest
There is no conflict of interests to declare.
Funding
This work is supported by NRF-2020R1A2C1013377 and NRF-2017R1D1A1B03030852 for H Seok.