Asthma predictive index as a useful diagnostic tool in preschool children: a cross-sectional study in Korea
Article information
Abstract
Background
It is challenging to diagnose asthma in preschool children. The asthma predictive index (API) has been used to predict asthma and decide whether to initiate treatment in preschool children.
Purpose
This study aimed to investigate the association between questionnaire-based current asthma with API, pulmonary function, airway hyperreactivity (AHR), fractional expiratory nitric oxide (FeNO), and atopic sensitization in preschool children.
Methods
We performed a population-based cross-sectional study in 916 preschool children aged 4–6 years. We defined current asthma as the presence of both physician-diagnosed asthma and at least one wheezing episode within the previous 12 months using a modified International Study of Asthma and Allergies in Childhood questionnaire. Clinical and laboratory parameters were compared between groups according to the presence of current asthma.
Results
The prevalence of current asthma was 3.9% in the study population. Children with current asthma showed a higher rate of positive bronchodilator response and loose and stringent API scores than children without current asthma. The stringent API was associated with current asthma with 72.2% sensitivity and 82.0% specificity. The diagnostic accuracy of the stringent API for current asthma was 0.771. However, no intergroup differences in spirometry results, methacholine provocation test results, FeNO level, or atopic sensitization rate were observed.
Conclusion
The questionnaire-based diagnosis of current asthma is associated with API, but not with spirometry, AHR, FeNO, or atopic sensitization in preschool children.
Key message
Question: Is physician-diagnosed current asthma in preschool children associated with the asthma predictive index, atopic sensitization, or pulmonary function test?
Finding: Physician-diagnosed current asthma in preschool children was associated with the asthma predictive index, but not with spirometry, methacholine provocation test, fractional expiratory nitric oxide level, and atopic sensitization.
Meaning: Physician-diagnosed asthma in preschool children may be different from classic atopic asthma in school children or adolescents.
Introduction
Asthma is the most prevalent chronic lower respiratory disorder in children worldwide [1]. The course of asthma varies from spontaneous remission to symptoms with repeated aggravation during the lifetime. The diagnosis of asthma and the control of its symptoms are very important, because asthma greatly influences public healthcare as well as a person’s quality of life [2].
Some factors, such as atopic dermatitis (AD), allergic rhinitis (AR), wheeze, and parental asthma are used as predictive risk factors, and several tests, including spirometry, fractional expiratory nitric oxide (FeNO), blood eosinophil counts, and methacholine provocation test, are known diagnostic tools for asthma [3]. However, the diagnosis of asthma in preschool children is very hard, because there is no golden standard for asthma diagnosis and the difficulty of performing some tests due to poor cooperations [1,4,5].
Spirometry, FeNO, methacholine provocation test, and bronchoalveolar lavage (BAL) can determine airway inflammation, airway hyperreactivity (AHR), and reversible airway obstruction; however, these cannot be performed reliably in younger children. Moreover, BAL is too invasive to perform in children. FeNO has been suggested as an indirect method for analyzing airway inflammation, but further research is needed to be widely used [5].
The asthma predictive index (API) was developed in 2000 using data from the Tucson Children’s Respiratory Study to predict the risk of asthma development at school age in preschool children. It has been used for screening high-risk groups for asthma development [5].
The purpose of this study is to determine the association of current asthma to the API and other laboratory tests such as spirometry, FeNO, AHR, and atopic sensitization test and verify the diagnostic accuracy of the API. Our findings will help identify children at risk of asthma and initiate early treatment in preschool children.
Methods
1. Study design
We performed a population-based, cross-sectional study involving 16 preschools in Seoul and Gyeonggi province, Korea. A total of 916 preschool children whose parents or guardians answered to the question regarding physician-diagnosed asthma and wheezing were enrolled. The questionnaire was based on the Korean version of modified International Study of Asthma and Allergies in Childhood questionnaire [6,7]. Children who had ever been diagnosed with asthma by physician and had any wheezing episode within the last 12 months before the questionnaire were categorized as “current asthma.”
To analyze the results, “recurrent wheeze” was defined as lifetime wheezes of 3 or more episodes based on the questionnaire. The “current” was defined as having symptoms or treatments within the last 12 months of answering the questionnaire, and “lifetime” was defined as having symptoms or treatments at any point in life.
Only children who could afford the tests and had not taken any medication or shown symptoms of respiratory infections within 1 month performed spirometry (n=482), FeNO (n=372), methacholine provocation test (n=212), and skin prick test (n=648). All tests were performed by the same well-trained technicians to ensure standardization of the results [8].
Outcome variables were the prevalence of allergic diseases, hospitalization or Emergency Department (ED) visit, atopic sensitization, blood eosinophil counts, serum IgE levels, forced expiratory volume in 1 second (FEV1), bronchodilator response (BDR), FeNO, and AHR and compared between preschool children with and without current asthma
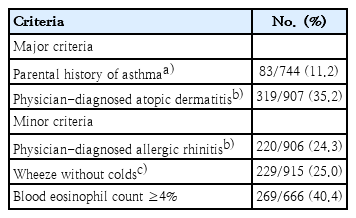
The API was assessed on the basis of factors in the questionnaire and blood eosinophil counts. (Table 1) [9]. The stringent index implies 3 or more wheezing episodes plus at least 1 major criteria or 2 minor criteria, and the loose index implies less than 3 episodes under the same conditions [5,9,10].
The study protocol was approved by the Institutional Review Board (IRB) of the University of Ulsan College of Medicine (IRB No. 2010-02 CON-14-P). Written consent was obtained after all the participants’ parents or guardians were provided sufficient information about the details of the study.
2. Fractional exhaled nitric oxide
FeNO was measured using a Niox Mino device (Aerocrine, Solna, Sweden) as described in a previous study [6,8]. The mean value of the 3 measurements was recorded as the final FeNO.
3. Pulmonary function test
Spirometry was performed using VMAX 22 (Sensormedics, Anaheim, CA, USA) as described in a previous study [11]. BDR was assessed by repeating the measurements 15 minutes after the inhalation of 200 mg of salbutamol [12], and a positive BDR was defined as a greater than 12% increase in FEV1 after bronchodilator inhalation.
4. Methacholine provocation test
Methacholine challenge tests were performed using the same method as described in a previous study [13]. AHR was defined when the concentration of methacholine required to induce a 20% decrease in FEV1 was lower than 8 mg/mL. The doseresponse slope was defined as the % decline of FEV1 divided by the final cumulative methacholine dose administered.
5. Measurement of serum total IgE concentrations and blood eosinophil counts
Serum total IgE concentrations were measured using an ImmunoCAP (ThermoFisher Scientific, Uppsala, Sweden). Blood eosinophil counts were obtained using an automatic blood cell counter (XE-100, Sysmex, Kobe, Japan). The results were converted to logarithmic values for analysis.
6. Atopic sensitization
A skin prick test (Allergopharma, Reinbek, Germany) using 16 common allergens (12 aeroallergens and 4 food allergens) was performed as previously mentioned [8]. The test was considered positive when the mean wheal size in response to an allergen was greater than 3 mm and at least equal to or greater than the mean wheal size in response to histamine. Atopic sensitization was defined as a positive skin prick test for any allergen.
7. Statistical analysis
Statistical analyses were performed using STATA ver. 11.0 (StataCorp LP, College Station, TX, USA). The mean values were compared between the 2 different groups by using Student t test. The significance of between-group differences in categorical variables between groups was tested using chi-square analysis.
Multivariate logistic regression was used to determine the associations of the API parameters with current asthma. Adjusted odds ratios and 95% confidence intervals were derived after adjusting for age, sex, height, and weight. All data were expressed as means±standard deviations or number (%), and significance was defined as a P value less than 0.05.
Results
1. Demographics and clinical characteristics of the study subjects
The mean age of the study subjects was 58.4 months, and 51.3 % were male. The prevalence of lifetime wheeze and recurrent wheeze was 25.0% and 13.3%, respectively. The prevalence of physician-diagnosed current asthma was 3.9% and the rate of physician-diagnosed lifetime asthma, AR, and AD was 8.4%, 24.3%, and 35.2%, respectively. Parental history of asthma was present in 11.2%. The rates of current and lifetime hospitalizations owing to wheezing were 14.4% and 43.3%, respectively. The rates of current and lifetime ED visits owing to wheezing were 10.1% and 29.0%, respectively (Table 2).
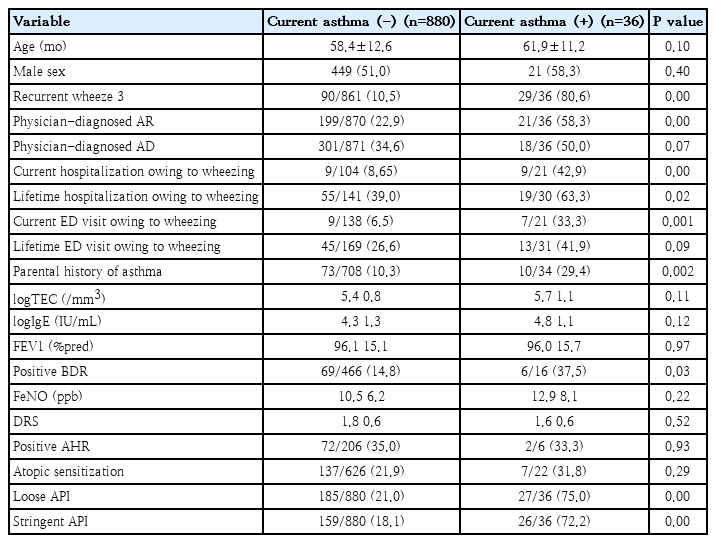
2. Comparison of clinical and laboratory parameters between children with and without current asthma
We compared the prevalence of allergic diseases, hospitalization or ED visit owing to wheezing, parental history of allergic diseases, and atopic sensitizations between the 2 groups. No significant differences were observed in age and sex. Children with current asthma showed a higher prevalence of physician-diagnosed AR. The prevalence of hospitalization and current ED visit owing to wheezing was higher in children with current asthma. Children with current asthma also had a higher rate of parental asthma and positive BDR. The proportion of positive APIs significantly increased in children with current asthma. However, no differences were observed in blood eosinophil counts, FeNO, AHR, and atopic sensitization between the 2 groups (Table 3).
3. Association of the API categories with current asthma
Multivariate logistic regression analyses were carried out to analyze the associations of the API with current asthma after adjusting for age, sex, weight, and height. The results showed that the API categories except for physician-diagnosed AD and blood eosinophil count ≥4% were significantly associated with current asthma. Both the stringent and loose APIs were associated with current asthma (Table 4).
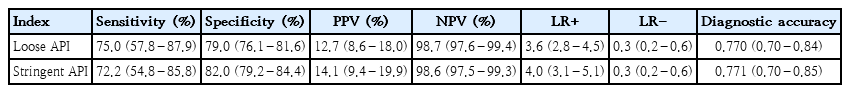
4. Diagnostic accuracy of the loose and stringent criteria for current asthma
The loose and stringent APIs showed 75.0% and 72.2% sensitivity, respectively, and 79.0% and 82.0% specificity, respectively, for current asthma. The loose and stringent APIs had high negative predictive values (NPVs) of 98.7% and 98.6%, respectively, but low positive predictive values (PPVs) of 12.7% and 14.1%, respectively. The positive likelihood ratio (LR+) and negative likelihood ratio (LR-) of the stringent API for current asthma were 4.0 and 0.3, respectively, and LR+ and LR- of the loose API were 3.6 and 0.3, respectively. The diagnostic accuracy of the loose and stringent APIs was 0.770 and 0.771, respectively (Table 5).
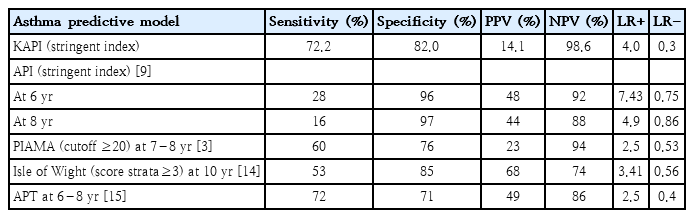
5. Comparison of the API to other predictive models
We compared the API in this study to other predictive models for asthma; the original API [9], the Prevention and Incidence of Asthma and Mite Allergy (PIAMA) risk score [3], Isle of Wight score [14], and asthma prediction tool (APT) [15] (Table 6). The API in this study showed higher LR+ and lower LR- compared to other predictive models for asthma except for the original API. The API in this study demonstrated the highest NPV and sensitivity compared to other predictive models, but lowest PPV.
Discussion
Several scoring systems have been developed to predict asthma, such as the API [1,9], PIAMA [3,4,16], Isle of Wight [14], modified API [17], APT [15], the severity score for obstructive airway disease [18], and an extension of the severity score [19]. The API, PIAMA, and APT were only validated in new populations. Among these, the API is the most useful predictor of the likelihood of asthma because it is simple and derives from unselected multiracial population [20]. To our knowledge, this is the first study to investigate the diagnostic utility of the API in preschool children in Korea. Unlike other prospective cohort studies, we used the data from a cross-sectional study and evaluated the diagnostic accuracy. The API from cross-sectional study was shown to be suitable to ascertain asthma status with 89.5% agreement rate and 0.66 kappa [21]. In this study, the stringent API showed 72.2% sensitivity and 82.0% specificity with a diagnostic accuracy of 0.771. The NPV was very high, suggesting that most children with a negative API may not have asthma. Our data showed that the API from cross-sectional study can be used as a diagnostic tool for asthma with reasonable accuracy in preschool children.
In our study, physician-diagnosed AD was not associated with current asthma. The allergic march begins with AD and AD is one of high-risk factors for asthma. Asthma is known to develop in 60% of children with severe AD and 20% with mild AD [22]. However, a retrospective analysis of 2 birth cohorts showed the proportion of children with both wheeze and eczema was only 5.8% [23]. In addition, while the prevalence of AD has doubled over the past decade, the prevalence of asthma has decreased by 50% in Korea [24]. The absence of increases in the prevalence of asthma has been observed globally, whereas the prevalence of AD and AR has seen a marked increase [24]. These findings indicate that the association between AD and asthma is relatively weak.
Parental history of asthma was significantly associated with current asthma in our study. This is supported by other studies that showed parental history of asthma to be a powerful risk factor for asthma in children [1,2,25]. Wheeze without cold was the most strongly associated with current asthma, as was recurrent wheeze. This may be in agreement with the findings of another study that showed frequent early wheeze to be the single most important predictor of asthma [10].
We also compared some test results, such as AHR, FeNO, and spirometry, between the 2 groups. Interestingly, current asthma was associated only with positive BDR, and not with atopic sensitization, AHR, FEV1, or FeNO. Asthma in preschool children may differ from late childhood or adult asthma [26]. Wheezing episodes are mostly episodic and triggered by viral infection, rather than by allergens. Moreover, there is less time for disease progression in preschool children; hence, airway obstruction demonstrating decreased FEV1 is uncommon. Preschool children show less airway inflammation, fixed airway obstruction, basement membrane thickening, and AHR than adults, even in severe cases [26].
In our study, current asthma was not associated with atopic sensitization, blood eosinophilia, and FeNO. Atopic sensitization has been found to be a risk factor for recurrent wheezing and associated with AHR [2,4], and eosinophilic inflammation can be predominant in patients with atopic sensitization. FeNO is associated with airway eosinophilic inflammation; it was significantly correlated with eosinophils and eosinophil cationic protein of sputum, airway mucosal biopsy, or BAL fluid in asthmatic patients [27,28]. Our results may be attributed to the fact that most preschoolers with wheezing are virus-induced, non-atopic and may not exhibit eosinophilic inflammation [29].
The prevalence of AHR, a typical characteristic of asthma assessed by the methacholine provocation test, showed no difference between the 2 groups in this study. Methacholine is a nonspecific direct stimulant acting on an airway smooth muscle receptor that results in bronchial constriction. Bronchoconstriction by methacholine is present not only in asthma but also in other acute and chronic airway inflammatory diseases [30]. Although AHR is the hallmark of asthma in older children and adults, a high frequency of negative methacholine test was reported in asthmatics [31]. In addition, young children may show different response to methacholine due to relatively underdeveloped airway and smooth muscle layer. A prospective study demonstrated that preschoolers who visited the ED owing to wheezing showed no difference in AHR from healthy preschoolers [32].
This study has some limitations. First, because this was a cross-sectional study, it was impossible to confirm whether the children developed asthma later. However, we calculated the diagnostic accuracy of the API and we can further obtain the prognostic accuracy of the API for asthma development. Second, it was a questionnaire-based study completed by the parents or guardians, not by physician chart reviews; therefore, recall bias or incorrect diagnosis may be present. However, questionnaire-based parent-reported wheezing showed a high agreement with physician-confirmed wheezing [33,34]. Finally, spirometry, bronchial provocation tests were difficult to perform in preschoolers since active cooperation is required [4], which results in a small number of testers. However, this is the source of efforts to develop biomarkers or asthma predictive models for asthma.
Although many biomarkers such as eosinophil-derived neurotoxin, eosinophil cationic protein, periostin, or exhaled breath condensate have been studied for the predictors of asthma, no indicator has as yet been confirmed as gold standard for diagnosis or prediction of asthma in preschool children. Furthermore, there have been no studies related to the API except for periostin. Serum periostin levels showed no difference in preschool wheezers according to the API [35]. The API is inexpensive, less invasive, and has been validated by several studies [5,20], and the diagnostic accuracy in this study is quite fair, so it can be used for asthma screening in preschool children. The strength of this study is that, unlike other studies, spirometry, AHR, FeNO, and BDR were evaluated in preschool children [20]. Together, our data is a population-based case-control study including mild asthma patients, unlike hospital-based studies including severe asthma patients. It can be applied to the other populations by representing the general population.
In conclusion, our results showed that the API was significantly associated with questionnaire-based current asthma in preschool children. The API may serve as a more reliable tool than spirometry, FeNO, methacholine provocation test, and atopic sensitization for diagnosing asthma in preschool children.
Notes
No potential conflict of interest relevant to this article was reported.