Strategies for treating and managing chronic hepatitis C in children in the direct-acting antiviral era
Article information
Hepatitis C virus (HCV) transmission occurs by the parenteral route [1]. In the early 1990s, after the commercialization of the anti-HCV enzyme-linked immunosorbent assay third-generation test, cases of HCV-infected children are rarely reported in Korea. The prevalence of HCV immunoglobulin G (IgG) positivity among Korean adolescents (age, 10–18 years) was 0.1% (2012–2014) according to the Korea National Health and Nutrition Examination Survey [2]. It is well known that HCV is not spread by casual contact. The main route of HCV infection in children is vertical transmission by infected mothers [1]. In the past decade, immigrants to Korea have increased; among them, some came from countries where HCV is more prevalent than in Korea. Furthermore, eyebrow tattoos are becoming popular; thus, pregnant women who opt for this procedure could become infected with HCV. Education about prevention is needed, especially regarding the routes of HCV transmission such as sharing of toothbrushes, razors, cutters, nail clippers, and unsterilized needles. There is currently no protective vaccine against HCV.
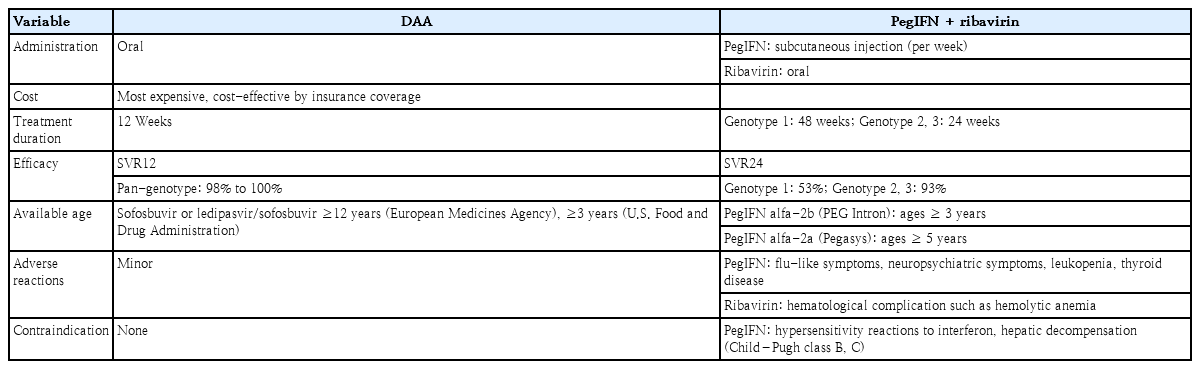
The framework for treating HCV infection is changing rapidly. New short-course oral direct-acting antiviral (DAA) drugs act directly on the HCV lifecycle and have very dramatic antiviral effects. Unlike interferon (IFN), DAA regimens has few contraindications and adverse reactions (Table 1). Since 2011, the U.S. Food and Drug Administration (FDA) and the European Medicines Agency have approved DAA regimens for the treatment of adults with chronic HCV infection. Both agencies approved DAA therapy (sofosbuvir or ledipasvir/sofosbuvir) for children (aged ≥12 years) in 2017. In 2019, both DAA were approved by FDA in pediatric patients aged 3 to less than 12 years. In June 2019, 12-week treatment with ledipasvir/sofosbuvir for any genotype was approved for Korean children (aged ≥12 years). Pediatric studies showed that DAA combination therapy is far superior to IFN-based therapies regardless of HCV genotype. In pediatric studies using the DAA regimen, the sustained virologic response at 12 weeks after treatment was 98%–100% in cases of approved DAA or currently in clinical trials [3]. Compared to studies of DAA in children with chronic HCV infection, the therapeutic efficacy of pegylated interferon (PegIFN) and ribavirin, measured by sustained virologic response at 24 weeks after treatment was 93% in patients with genotype 2 or 3, 80% in patients with genotype 4, and only 53% in those with genotype 1 [4].
In the current issue of the journal, Rashed et al. [5] investigated thyroid dysfunction in children with HCV infection receiving PegIFN plus ribavirin and showed that 28% of children (14 of 50) developed subclinical hypothyroidism. PegIFN-based therapies have various burdensome adverse reactions such as thyroid dysfunction. The incidence of thyroid dysfunction increases to 15%–40% with IFN use [6]. The types of thyroid dysfunction were subclinical hypothyroidism (50.7%), and so on such as hypo-, hyper-, and subclinical hyperthyroidism and thyroiditis [7].
The approval of DAA for use in children is in progress in several countries but still not allowed in many countries. IFN-based therapies are still widely used for treating children worldwide. Although PegIFN plus ribavirin is approved for children with HCV infection (age ≥3 years), IFN treatment is no longer recommended for children in the DAA era except for a few with significant morbidity by rapid progression such as the occurrence of advanced fibrosis [1,8]. Deferring IFN treatment is recommended until DAA regimens are approved for children (aged <12 years) because HCV-related liver disease occurs infrequently in children [1,8]. In the near future, if DAA is available, it can be used for all HCV-infected children (≥3 years of age) independent of disease severity [1,9]. According to a recent guideline for HCV in children, anti-HCV IgG levels should be determined for all children (≥18 months of age) born to HCV-infected women, HCV-RNA polymerase chain reaction should be considered in the first year of life for perinatally exposed children, and screening should be repeated after 3 years of age in cases of anti-HCV positive results (≥18 months of age). Liver enzymes should be checked at the initial appointment and then annually thereafter, and a severity assessment is required [9].
Notes
No potential conflict of interest relevant to this article was reported.