A pediatric case of idiopathic Harlequin syndrome
Article information
Abstract
Harlequin syndrome, which is a rare disorder caused by dysfunction of the autonomic system, manifests as asymmetric facial flushing and sweating in response to heat, exercise, or emotional factors. The syndrome may be primary (idiopathic) with a benign course, or can occur secondary to structural abnormalities or iatrogenic factors. The precise mechanism underlying idiopathic harlequin syndrome remains unclear. Here, we describe a case of a 6-year-old boy who reported left hemifacial flushing and sweating after exercise. He had an unremarkable birth history and no significant medical history. Complete ophthalmological and neurological examinations were performed, and no other abnormalities were identified. Magnetic resonance imaging was performed to exclude lesions of the cerebrum and cervicothoracic spinal cord, and no abnormalities were noted. His final diagnosis was classic idiopathic harlequin syndrome. Herein, we report the first pediatric case of idiopathic harlequin syndrome in Korea.
Introduction
Harlequin syndrome (HS) is an uncommon disorder of the sympathetic nervous system characterized by unilateral diminished flushing and contralateral sweating of the face in response to heat, exercise or emotional stimuli12). More than 100 cases have been reported in the literature since the initial description of HS by Lance et al. in 19883). Most reported cases of HS are primary (idiopathic) in which no underlying etiology could be identified, and HS is more commonly seen in female4). In contrast, most of the reported cases of HS in children have been heterogeneous secondary causes5). However, the precise mechanism of idiopathic HS is still unclear4).
HS is a clinically remarkable disorder rarely encountered in the pediatric practice. Although this disorder is usually benign and does not need any specific treatment, physicians should consider performing a detailed clinical examination, testing autonomic functions, and conducting appropriate imaging techniques to find underlying organic causes5). To our knowledge, only a few adult patients have been reported from Korea6). We report a pediatric case of idiopathic HS in a 6-year-old boy.
Case report
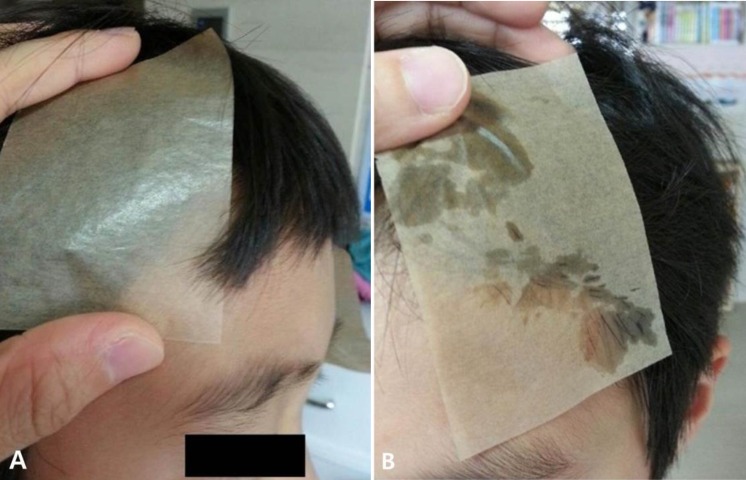
A 6-year-old boy visited the pediatric outpatient clinic, complaining of unilateral hemifacial flushing and sweating occurring within minutes during or after physical exercise or heat. Over the past 2 years, these episodes had occurred as an isolated symptom without any change in severity. He had an unremarkable birth history and uneventful medical history for trauma or surgery. Additionally, he did not take any medications. None of his family members had similar symptoms. His neurological examination showed normal findings, including normal pupil responses, cranial nerve functions, and muscle stretch reflexes. The rest of systemic examination was unremarkable. His blood pressure and heart rate were normal, and no signs of asymmetric flushing or sweating at rest were noticed. Electrocardiographic findings were within normal limits. Laboratory tests, including the white blood count; levels of hemoglobin, glucose, and electrolytes; and renal, liver, and thyroid function were normal. To objectify hemifacial flushing and sweating, we performed a provocation test (i.e., running for 90 seconds in direct sunlight outdoors). After exercise-induced sweating, there was pale and nearly complete anhidrosis on the right side of the face with compensatory hyperhidrosis and flushing on the opposite side with sharp demarcation (Fig. 1). By using an oil control film, we found that the oil-paper firmly stuck to the left side of the patient's face owing to sweating, but that it immediately slipped off the right side of his face (Fig. 2). On ophthalmological examination, he had mild anisocoria. The right pupil was 1.5 mm in size, while the left pupil was 2.5 mm in size; however, no ptosis, miosis, or enophthalmos was noted, and both pupils responded normally to light and accommodation. Subsequent testing showed no evidence of Horner's syndrome. Magnetic resonance imaging (MRI) was performed to exclude lesions in the cerebrum and cervicothoracic spinal cord, and no abnormalities were noted. In summary, the clinical picture was compatible with idiopathic HS. The child and his parents were explained the benign nature of this condition, and we advised regular follow-ups without medication.
Discussion
Classically, HS is defined as unilateral facial flushing and sweating with normal ocular sympathetic innervation, but it has been gradually considered a spectrum of partial dysautonomias affecting sudomotor, pupillary, and vasomotor responses in the facial or facio-brachial region5). The nonflushing side of the face has autonomic dysfunction, while the flushing side of the face has normal autonomic function. The sympathetic hyperactivity of the flushing side may be a kind of compensatory reaction that provides normal heat regulation of the whole face17). Although listed as a rare disease, HS has been reported more widely in the literature in the past 20 years, particularly in adults124567). Since 1990, pediatric cases of HS have been sporadically published in other countries; however, this is the first pediatric case in Korea, except for that reported in a newborn.
The exact pathophysiology of axonal damage or degeneration in primary HS is still unknown. Congenital HS is regarded as a sympathetic autonomic dysfunction in the control of peripheral capillary bed tonus, probably because of the hypothalamic functional immaturity in the newborns8). Some authors have suggested that an anterior radicular artery at the third thoracic segment is occluded during strenuous exertion3) or asymmetric migration of the neural crest cell occurs during embryogenesis, but these cannot explain the symptom arising in adulthood9). Conversely, others have speculated that microvascular ischemia mediated by an autoimmune process or infectious agent such as the herpes simplex virus, cytomegalovirus, and parvovirus and human herpes virus 6 may be responsible79). The latter point is more acceptable in pediatric HS.
The dysfunction seen in this disease, even though it is predominantly idiopathic, occurs by an alteration of sympathetic nervous system activity, secondary to the lesion of the preganglionic fibers, and superior cervical ganglion or postganglionic fibers in the external carotid plexus such as the brainstem infarct and superior mediastinum neurinoma6). In addition, most cases of iatrogenic HS have been reported to be caused by injury of the sympathetic nervous system and neural damage at T2 or T31). Iatrogenic HS has also occurred after endoscopic surgery for the removal of a solitary pulmonary nodule, internal jugular vein catheterization, paravertebral thoracic anesthetic block, surgical resection of a neck mass, and thoracic sympathectomy1011). In addition, unlike many adults, most of the reported cases of HS in children have been secondary5), and if present at birth, it may be associated with Horner's syndrome2). A previous report presented 10 cases of asymmetric facial flushing in childhood and adolescence2), and among them, 8 had organic lesions or structural defects, with 4 having preganglionic Horner's syndrome and one having postganglionic neuronal degeneration. The lesions included a neurinoma in the mediastinum, a cystic hygroma in the right neck, and a cervical neck mass. Moreover, 2 cases had unknown causes, and only 1 case had no lesion.
A diagnosis of HS is made on the basis of clinical observations and examination findings. The neurons controlling sweating and blood flow in the face have been shown to innervate the same pupillary muscles; therefore, damage to these muscles or the area around these muscles may result in dysfunction of the neurons2). These partial dysautonomias may indicate other diseases such as Horner's syndrome, Adie's syndrome, and Ross' syndrome5). Horner's syndrome is characterized by miosis, ptosis, enophthalmos, and anhidrosis, and these symptoms occur on the same side as that of the nerve injury1213). Adie's syndrome, also known as Holmes-Adie's syndrome or Adie's tonic pupil, is a neurological disorder characterized by a tonically dilated pupil that reacts slowly to light but shows a more definite response to accommodation14). Ross' syndrome involves Adie's syndrome along with segmental anhidrosis4). When a patient has the harlequin sign, it is important to rule out traumatic causes, identify other possible causes, and perform the autonomic function test to provide appropriate treatment. The symptoms of autonomic dysfunction include orthostatic hypotension, abnormal sweating, urinary incontinence, and irregular papillary movement. An autonomic function test is noninvasive and easy to perform, and can be used to detect autonomic dysfunction. The autonomic function test includes the tilt table test, orthostatic blood pressure measurement, head-up test, Valsalva maneuver, thermoregulatory sweat test, and electrocardiography15). An autonomic function test is necessary to rule out other causes of HS; but it is difficult to perform in a young child. Reluctantly, we performed the provocation test for increasing body temperature by vigorous exercise instead of the treadmill test in this patient. Further examinations such as MRI of the brain and spinal cord, MRI angiography of the carotid arteries and imaging of the region adjacent to the stellate ganglion may be performed to distinguish between primary and secondary forms5).
When a clinician encounters a patient with hemifacial flushing or sweating, the medical history of the patient should be carefully taken, and complete neurological and ophthalmological examinations should be performed. Primary HS does not involve structural abnormalities, and it can be either congenital or idiopathic. Idiopathic HS has a benign course, and therefore, medical treatment is not required; however, counseling can be provided to the patient, and regular follow-up should be suggested. Contralateral sympathectomy may be performed in patients with severe discomfort. Surgical intervention may be performed in patients with structural lesions; however, this should be carefully considered as it may result in other complications4). To our knowledge, a clinical presentation of idiopathic HS in children has not been previously reported in Korean pediatric literature. We hope that this report will make pediatricians aware of this rare syndrome.
Notes
Conflict of interest: No potential conflict of interest relevant to this article was reported.